Royal London
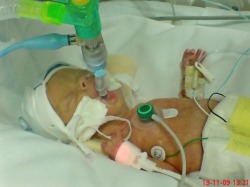
Getting bigger - slowly
........ And so it was that Ethan went to Royal London hospital. I was stronger by then and so we made the trip by train. The Royal London's visiting rules was Parents only - which is similar to Lutons so again only me and his Father could see him. His Grandmother had seen Ethan at birth but that was it! Ethan was very poorly but they wanted to wait before doing any surgery on his stomach, mainly because his lungs were so weak and they wanted to deal with the breathing then deal with the stomach issue. I remember having a conversation with one of the doctors Mike, who was explaining how poorly Ethans lungs was. I asked "can you fix him?" and he answered "I think so". At that time that is all I wanted to know.
One of the worst conversations was with a particularly pessimistic doctor who explained his lungs were very very bad, and he was worried about his tummy and that if he did need surgery it would be 50/50. Well we were walking on a tightrope any way but the news upset me a lot - for a while. Again not a lot I could do about anything so nothing to do but sit and wait, and hope! It was at this point that Ethan's father felt he could not cope, so his visits were few and far between.
The Royal London was closer to home then Luton for sure, however what with the other children and the financial cost of travel (neither of us drive) I could only get to the hospital 4/5 days a week, on my own as Ethans Father found it hard to cope, which I hated. However the other few days I did manage some sort of normality and it was key to getting my strength back. This of course changed as Ethan was "woken" up and I did end up spending 7 days a week at the hospital, or as much as I could afford to that week!
As time went on and the days and the weeks moved on I started to research more about the machines, about the medications and about prematurity in general. This helped as I was no longer scared as much, I find I am scared more about the unknown then I am if I know what I am looking at. I really think research and lots of question asking can really help if you are that way inclined.
Back to The London and Ethan was not really putting on weight and the feeding issue was not resolved so he was still on TPN, which is food fed direct into the blood stream but long term can be toxic. (He did eventually go into liver failure due to TPN) After a course of steroids he was moved off the ventilator and onto to CPAP.
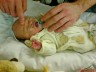
I was elated at the news! So beyond happy, my boy was making progress. I had my first cuddle without the ventilator, I saw his face when they washed him, I was walking on air. The first cuddle I had with him at that time he was so small, it seemed that he did not weigh anything at all. His SATS - or the amount of oxygen in his blood dropped to high 60's so I had to put him back.
For a few days all I could do was lower the cot bed and sit with him. After 7 days I had a call to say his lungs were not strong enough and he had to be re-ventilated. I understood then the "rollercoaster" of emotions.
By December as it became apparent that Ethan was going to be ventilated for a long time we were allowed to cuddle Ethan while he was Ventilated, I loved those cuddles but we were so afraid of moving him and knocking his ventilator tube!
I was frustrated that no surgery had happened but yet Ethan was not being fed either. I called a meeting with a consultant and I explained my frustration, Ethans settings had not changed, his weight had not changed and we were going no where. The consultant explained that they wanted Ethan to be stronger then he was before doing the surgery, my thoughts being - how could he get stronger without the surgery?
However the very next day I got a phone call to say they were going to do the surgery that day, as after speaking to me the day previous they realised they were waiting for nothing and the operation must be done at some point. Their focus changed from lungs to stomach and maybe sorting out feeding and therefore allowing him grow will help his lungs. It was the only chance he had! I spent hours with Ethans grandmother (who came to sit with me as his father did not want to) waiting for Ethan to come out of surgery, I was so pleased to see him when he did and the surgeon explained that she had left 45 cm of bowel left, crucially the Ileocrcal Valve was left in tact as was the ileum ( this being an important role in absorbing feeds), the rest was damaged and all bunched up together, Ethan had had NEC, the infection had gone but had left damage. Ethan had a stoma bag which means the two open ends of his bowel were brought to the outside of his body and the waste was collected in a bag on his stomach. It wasnt as scary looking as I thought, like red sausages!
The stoma bag was a pain and Ethan did not like it very much as he kept pulling on it. This meant he would loosen the seal around the bag and when I had him out for a cuddle twice he leaked all over me! Once the nurse turned her back only to look at him again and Ethan had the Stoma bag in his hand and was waving it at her, covering him and the incubator in poo!
Ethan was slowly introduced to milk, but the stoma out put was still high as he was not absorbing the milk very well. This meant he was still on the TPN which was causing him liver failure. Again I was desperate to get the Stoma closed to see if that would help the absorption. Interestingly when he came out of the first surgery his ventilator setting immediately dropped from 80% O2 to 35%. It shows how much the stomach can affect breathing! However he was only on minimal amount of milk, and I was worried that if he could not tolerate food and therefore grow properly - his future was not looking good.
8 weeks after Ethan had his NEC surgery he had his stoma reversal surgery. This time as it was scheduled operation, I arrived early (as told it would be at 8.30am) only to be told it would be delayed by a few hours and then to be told it was not happening that day. I had made friends with a few other mothers in the NICU and one of them I am still close to, Irene and her baby girl Angelina. I spent the day with Ethan and went for a late lunch with Irene and when I came back was told he was going for his surgery after all! Thank you to Irene for staying with me and talking rubbish with me! Again the surgery went well with nothing else taken away. I would have to wait 10 days before feeding would recommence before we knew if he could tolerate feed!
I must thank his surgeon who I believe was called Georgina and Niall, Georgina for her wonderful drawings and for taking me under her wings. Allowing me to take Ethan to theatre and to collect him as well, plus the nurses who thought I was a bit mad when I grabbed a random porter to take Ethan back to the NICU as I did not want to wait soooo long for a porter!
Thankfully he did tolerate feed and slowly but surely his feed went up and he did a POO, his first ever! I was so pleased and have never been so pleased about poo in my life! I would have taken a picture of it, that is how excited I was but realised that was going slightly too far!
As he got stronger his ventilator settings went down, by now I had learnt every thing I could about ventilators and so could read the ventilator and all of the machines like a pro! Then just after xmas (which was a nightmare as the trains did not run for 2 days!) I had the best news! Ethan was back on CPAP!
He hated CPAP and I was told a long road lay ahead of us, but at least it was not the ventilator and for the first time I could hear him cry, a proper cry and not the tiny little murmurs I heard when he first went on to CPAP! (Which I recorded and his nurse made me laugh by saying to Ethan , come on baby cry for mummy!) A childs cry is a wonderful sound! I wish I had that video still.
Not long after this I walked in to see that he was in his incubator but the lid was off as he was now big enough to regulate his own temperature. We also found out that Ethan had brittle bone disease of prematurity and had broken his own leg :( that made nappy changes changeling!
It was only a few weeks after this that Ethan was moved out of the NICU and into the HDU! In the HDU I could do more for Ethan and get him in and out of the cot by myself, plus he could wear clothes!!! Cue loads of shopping! It also meant I could give him his first proper bath!
By the end of January Ethan was on nasal cannula and doing very well! It meant I got to see Ethans hair and his face for the first time as he was taken off the CPAP hat! His hair was all messy as he had had an EEG (brain electrobe test) which left all the muck on hair. Ethan smelt of biscuits and "stuff" as he was so poorly he had been unable to have a bath!
Through most of this Ethan had to have an almost constant infusion of antibiotics as he had many infections, many severe and many life threatening. Again there was nothing I could do but sit and hope but he fought back all the time. He did have countless blood transfusions, I was so used to being told that he had to another I took it my stride!
He was constantly reviewed for ROP by the eye doctor as too much O2 can make the blood vessels around the retina grow too much and potentially detatch the retina from the eye! Ethan was threatened surgery week after week but thankfully did not need it!
It was at this time I was able to give Ethan his first bathtime and a moment in which I finally felt like a real mum.
By February we were given the wonderful news that Ethan was well enough to be transferred to the local hospital! He was off continuous feeds and on hourly feeds at this point and though he seemed to have an issue with reflux things were on the up!
At the last minute I was told Ethan could not be transferred as they did not have the staff. I phoned Southend Hospital myself and spoke to the ward, "we dont have the staff to take another baby on CPAP" I was told. "Ethan is not CPAP" I replied!! So off we went after all!
I stayed with Ethan all night to make the journey by ambulance with him and arrived back at home at 2am! I was shattered but it was nice to know that I could get up and walk to go and see him. Even better the other children could now meet their baby brother for the first time! This also made me panic about infections and kids sniffing etc so almost constant hand washing has now been introduced to every one in the household whether we are at the hospital or not!
THANK YOU to everyone at Royal London Elizabeth ward Dr Nik Cholidis and Dr Mike Hird especially. Massive thank you to Irene for her support.
One of the worst conversations was with a particularly pessimistic doctor who explained his lungs were very very bad, and he was worried about his tummy and that if he did need surgery it would be 50/50. Well we were walking on a tightrope any way but the news upset me a lot - for a while. Again not a lot I could do about anything so nothing to do but sit and wait, and hope! It was at this point that Ethan's father felt he could not cope, so his visits were few and far between.
The Royal London was closer to home then Luton for sure, however what with the other children and the financial cost of travel (neither of us drive) I could only get to the hospital 4/5 days a week, on my own as Ethans Father found it hard to cope, which I hated. However the other few days I did manage some sort of normality and it was key to getting my strength back. This of course changed as Ethan was "woken" up and I did end up spending 7 days a week at the hospital, or as much as I could afford to that week!
As time went on and the days and the weeks moved on I started to research more about the machines, about the medications and about prematurity in general. This helped as I was no longer scared as much, I find I am scared more about the unknown then I am if I know what I am looking at. I really think research and lots of question asking can really help if you are that way inclined.
Back to The London and Ethan was not really putting on weight and the feeding issue was not resolved so he was still on TPN, which is food fed direct into the blood stream but long term can be toxic. (He did eventually go into liver failure due to TPN) After a course of steroids he was moved off the ventilator and onto to CPAP.
I was elated at the news! So beyond happy, my boy was making progress. I had my first cuddle without the ventilator, I saw his face when they washed him, I was walking on air. The first cuddle I had with him at that time he was so small, it seemed that he did not weigh anything at all. His SATS - or the amount of oxygen in his blood dropped to high 60's so I had to put him back.
For a few days all I could do was lower the cot bed and sit with him. After 7 days I had a call to say his lungs were not strong enough and he had to be re-ventilated. I understood then the "rollercoaster" of emotions.
By December as it became apparent that Ethan was going to be ventilated for a long time we were allowed to cuddle Ethan while he was Ventilated, I loved those cuddles but we were so afraid of moving him and knocking his ventilator tube!
I was frustrated that no surgery had happened but yet Ethan was not being fed either. I called a meeting with a consultant and I explained my frustration, Ethans settings had not changed, his weight had not changed and we were going no where. The consultant explained that they wanted Ethan to be stronger then he was before doing the surgery, my thoughts being - how could he get stronger without the surgery?
However the very next day I got a phone call to say they were going to do the surgery that day, as after speaking to me the day previous they realised they were waiting for nothing and the operation must be done at some point. Their focus changed from lungs to stomach and maybe sorting out feeding and therefore allowing him grow will help his lungs. It was the only chance he had! I spent hours with Ethans grandmother (who came to sit with me as his father did not want to) waiting for Ethan to come out of surgery, I was so pleased to see him when he did and the surgeon explained that she had left 45 cm of bowel left, crucially the Ileocrcal Valve was left in tact as was the ileum ( this being an important role in absorbing feeds), the rest was damaged and all bunched up together, Ethan had had NEC, the infection had gone but had left damage. Ethan had a stoma bag which means the two open ends of his bowel were brought to the outside of his body and the waste was collected in a bag on his stomach. It wasnt as scary looking as I thought, like red sausages!
The stoma bag was a pain and Ethan did not like it very much as he kept pulling on it. This meant he would loosen the seal around the bag and when I had him out for a cuddle twice he leaked all over me! Once the nurse turned her back only to look at him again and Ethan had the Stoma bag in his hand and was waving it at her, covering him and the incubator in poo!
Ethan was slowly introduced to milk, but the stoma out put was still high as he was not absorbing the milk very well. This meant he was still on the TPN which was causing him liver failure. Again I was desperate to get the Stoma closed to see if that would help the absorption. Interestingly when he came out of the first surgery his ventilator setting immediately dropped from 80% O2 to 35%. It shows how much the stomach can affect breathing! However he was only on minimal amount of milk, and I was worried that if he could not tolerate food and therefore grow properly - his future was not looking good.
8 weeks after Ethan had his NEC surgery he had his stoma reversal surgery. This time as it was scheduled operation, I arrived early (as told it would be at 8.30am) only to be told it would be delayed by a few hours and then to be told it was not happening that day. I had made friends with a few other mothers in the NICU and one of them I am still close to, Irene and her baby girl Angelina. I spent the day with Ethan and went for a late lunch with Irene and when I came back was told he was going for his surgery after all! Thank you to Irene for staying with me and talking rubbish with me! Again the surgery went well with nothing else taken away. I would have to wait 10 days before feeding would recommence before we knew if he could tolerate feed!
I must thank his surgeon who I believe was called Georgina and Niall, Georgina for her wonderful drawings and for taking me under her wings. Allowing me to take Ethan to theatre and to collect him as well, plus the nurses who thought I was a bit mad when I grabbed a random porter to take Ethan back to the NICU as I did not want to wait soooo long for a porter!
Thankfully he did tolerate feed and slowly but surely his feed went up and he did a POO, his first ever! I was so pleased and have never been so pleased about poo in my life! I would have taken a picture of it, that is how excited I was but realised that was going slightly too far!
As he got stronger his ventilator settings went down, by now I had learnt every thing I could about ventilators and so could read the ventilator and all of the machines like a pro! Then just after xmas (which was a nightmare as the trains did not run for 2 days!) I had the best news! Ethan was back on CPAP!
He hated CPAP and I was told a long road lay ahead of us, but at least it was not the ventilator and for the first time I could hear him cry, a proper cry and not the tiny little murmurs I heard when he first went on to CPAP! (Which I recorded and his nurse made me laugh by saying to Ethan , come on baby cry for mummy!) A childs cry is a wonderful sound! I wish I had that video still.
Not long after this I walked in to see that he was in his incubator but the lid was off as he was now big enough to regulate his own temperature. We also found out that Ethan had brittle bone disease of prematurity and had broken his own leg :( that made nappy changes changeling!
It was only a few weeks after this that Ethan was moved out of the NICU and into the HDU! In the HDU I could do more for Ethan and get him in and out of the cot by myself, plus he could wear clothes!!! Cue loads of shopping! It also meant I could give him his first proper bath!
By the end of January Ethan was on nasal cannula and doing very well! It meant I got to see Ethans hair and his face for the first time as he was taken off the CPAP hat! His hair was all messy as he had had an EEG (brain electrobe test) which left all the muck on hair. Ethan smelt of biscuits and "stuff" as he was so poorly he had been unable to have a bath!
Through most of this Ethan had to have an almost constant infusion of antibiotics as he had many infections, many severe and many life threatening. Again there was nothing I could do but sit and hope but he fought back all the time. He did have countless blood transfusions, I was so used to being told that he had to another I took it my stride!
He was constantly reviewed for ROP by the eye doctor as too much O2 can make the blood vessels around the retina grow too much and potentially detatch the retina from the eye! Ethan was threatened surgery week after week but thankfully did not need it!
It was at this time I was able to give Ethan his first bathtime and a moment in which I finally felt like a real mum.
By February we were given the wonderful news that Ethan was well enough to be transferred to the local hospital! He was off continuous feeds and on hourly feeds at this point and though he seemed to have an issue with reflux things were on the up!
At the last minute I was told Ethan could not be transferred as they did not have the staff. I phoned Southend Hospital myself and spoke to the ward, "we dont have the staff to take another baby on CPAP" I was told. "Ethan is not CPAP" I replied!! So off we went after all!
I stayed with Ethan all night to make the journey by ambulance with him and arrived back at home at 2am! I was shattered but it was nice to know that I could get up and walk to go and see him. Even better the other children could now meet their baby brother for the first time! This also made me panic about infections and kids sniffing etc so almost constant hand washing has now been introduced to every one in the household whether we are at the hospital or not!
THANK YOU to everyone at Royal London Elizabeth ward Dr Nik Cholidis and Dr Mike Hird especially. Massive thank you to Irene for her support.